Summary
Covid-19 (the infection outcome of the SARS-Cov_2 virus) is here to stay, for a period measured in years, rather than weeks or months, as this Nature article discusses.
That is even if a significantly new variant doesn’t appear. It is entirely possible: there have already been some further sub-variants of Omicron, particularly in South Africa, although they haven’t yet developed to threaten the current dominance of Omicron BA.2 in the UK.
There are five variants in my current model: since the original, I have added Alpha, Delta, Omicron BA.1 and BA.2, each of which has shown significant bumps in cases and deaths as they supplant the previous one(s). As no new variant is currently threatening in the UK, even though one may be discovered at any time, it would be pure speculation to postulate a particular date for any new one in my model.
In this article, therefore, I will present a few variations of the model with different assumptions about the UK’s current dominant variant, Omicron BA.2. The outcomes are fairly consistent over the 1400 day period of the model, from the outset in February 2020, to December 2023, and show that as NPIs are removed, vaccination is what keeps us safe.
The view of experts in the field
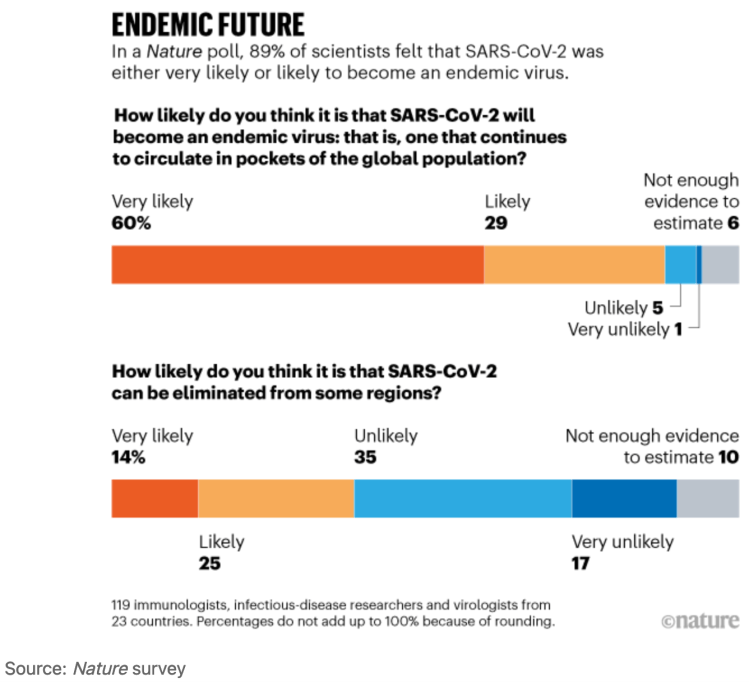
The Nature article I referred to above presents a summary chart of the opinions of more than 100 immunologists, infectious disease researchers and virologists working on the coronavirus as to whether it could be eradicated.
As the following chart indicates, almost 90% of expert respondents thought that the coronavirus will become endemic — meaning that it will continue to circulate in pockets of the global population for years to come.
The ZOE Project
A corroborating opinion is provided by Prof Tim Spector of King’s College London, who co-founded the ZOE project in March 2020 to collect and analyse data on Covid-19 incidence (daily new cases) and prevalence (% penetration into the UK population). I contribute through the ZOE app on my iPhone as one of nearly 5 million people in the UK making daily returns on our health and Covid status.
Prof Spector publishes a weekly YouTube video on ZOE findings on the pandemic; see this week’s video presentation here for his current outlook. In these videos, he explains his view of the current Covid situation in the UK, and some of the influencing factors, as well as other related health matters including diet and nutrition.
His message this week is not only that Covid-19 isn’t over by any means, but also that official published statistics on incidence (daily new cases) might be seriously underestimated.
Prof Spector asserts that according to his analysis of our ZOE app returns vs. Government data provided by the Office for National Statistics (ONS), official reported data on Covid incidence (new cases) might currently be underestimated by a factor of six – 40,000 reported per day at present, instead of 230,000 new cases per day as shown by the ZOE analysis of returns from its 5m users.
This would tend to explain why my model charts that you will see later, comparing published UK data to my model forecasts, fit the reported Deaths data very well, but currently overestimate the reported Active Case numbers.

Prof Spector wonders if the the under-reporting is because LFT tests are no longer free (in England, the largest of the UK home country populations), and can no longer be uploaded, so that official statistics are understated as a result.
He also notes that incidence of Covid-19 is falling faster in Scotland than in the other home countries, as he showed on the following chart in the video.

It might just be coincidence that LFT test kits, although now chargeable in England, remain free in Scotland until the end of April, and that advice on mask wearing and other personal precautionary measures has been and remains more conservative in Scotland than elsewhere.
Further variants?
Prof Tom Wenseleers, at the University of Leuven, is already publishing material on Twitter (as many academics do nowadays) about Omicron BA.4 and BA.5 in South Africa, although distinguishing, in his Twitter thread, the situation there, where vaccination rates are low, from here in the UK where they are high.
He says “The BA.4 & BA.5 Omicron subvariant-driven increase of new confirmed Covid cases in South Africa gives a good idea of what the endemic equilibrium will look like: a significant wave every 6 months with significant mortality & morbidity.”
But he also says “The cumulative number of infections that the UK saw, per the ONS infection survey results, may be roughly similar. But there is one major difference: a decent vaccine rollout & uptake greatly reduced Covid mortality compared to SA, where only 30% are fully vaccinated & 4% bolstered.”

Prof Wenseleer’s comments are words to the wise: it is far from clear the pandemic is over, especially as it is a worldwide issue, and we aren’t safe until everyone is safe.
The importance of vaccination when reducing NPIs
My previous modelling of Covid-19 , which I have reported in around 50 blog posts since March 2020, has demonstrated the way in which the successful programme of vaccination in the UK has allowed Non Pharmaceutical Interventions (NPIs), comprising the different elements of the various lockdowns we have endured, to be reduced.
The first of my articles on vaccination on November 18th 2020, just prior to the launch of vaccination in December 2020, was followed by many others, and in February 2021 Prof Alex de Visscher, Dr Tom Sutton and I published our paper “Second-wave Dynamics of COVID-19: Impact of Behavioral Changes, Immunity Loss, New Strains, and Vaccination” where we explored the impact of vaccination in a theoretical situation, supported by modelling in the UK context.
All my subsequent work has confirmed the positive impact of vaccination. In the NPI reduction examples that follow, I present comparative model outcomes where I remove modelled NPIs in stages on 24th February 2022, culminating in the removal of all NPIs.
NPIs and legal powers
Most legal NPI restrictions were removed in England 24th February 2022, with the few remaining ones, such as mask-wearing in confined public spaces and on public transport, and self-isolation after infection, becoming advisory. Other home countries of the UK have taken similar actions, although at somewhat different times.
Northern Ireland did this on February 15th 2022; in Wales, most regulations were removed on 28 March, but in response to rising case numbers, face-coverings were again required from April 18th. Assuming the situation remains stable, however, legal restrictions will be removed in Wales on May 9th. In Scotland, from where I write this blog, legal restrictions were removed this week, on Monday 18th April 2022. This timing prompted me to write this article now.
In all cases, some advisory restrictions remain, but over the past two years and more, it has been a complex and moving situation, with different mitigations (NPIs) taking effect and being removed at different times in the four home countries, in response to arrivals of the different variants.
NPI representation in my model
In the model, I have represented the NPIs, following the first full UK lockdown imposition on March 23rd 2020, by percentage increments or decrements in aggregate NPI effectiveness. In the model, this starts with that first March 23rd 2020 lockdown at 84.3% NPI effectiveness, which results in death and case rates in the model matching reality at that time. At that date, therefore, the virus transmission rate in the model was reduced to 15.7% of what it would have been without any NPIs or modified behaviour on the part of the public.
The successive NPI adjustments are tabulated in all of my model charts, and the latest adjustment on February 24th 2022, testing the outcomes and forecasts in the model, removes restrictions in percentage steps, via several scenarios, culminating in a -79.64% reduction, which removes all remaining restrictions and public behavioural precautions in the model.
This total NPI and behavioural precautions removal could be seen as a step too far, because many in the UK population, depending on demographic factors such as age, have continued, at some level, voluntarily to restrict their travel, work and social arrangements to minimise contact rates with others. But I have also run several other, lower NPI/ behavioural effectiveness reductions (-8%, -15%, -30% and -50%), and, such is the positive impact of vaccination, the percentage differences in December 2023 outcomes in Active Cases and cumulative deaths were not large, as we shall see.
In my 23rd November 2021 article, when modelling the implications of “Freedom Day” (July 19th 2021), I highlighted the average contacts per day per individual in July 2021 as reported by the BBC at about 4, compared with 10 pre-pandemic, which would be consistent with reduced infection transmission rates experienced at that time, and shows the propensity for the public in general to be responsible in the face of the pandemic.
It is probably the case, therefore, that less than a total removal of modelled NPIs might better reflect the real situation, and hence the reason for my running several parametric stages of NPI reduction.
I also remarked in that November 2021 article that “…most professional modellers in the UK have been surprised that infection rates have been fairly low so far, following the July 19th “Freedom Day” removal of all lockdown measures, compared with their expectations. Some of their prior expectations of 100,000 cases per day seemed very high to me.“
I expect that was also the result of the effectiveness of the vaccination programme in that period, aimed at the most vulnerable and oldest parts of the population, which had been running for seven months by then.
Introduction to model setup – age groups and vaccination
As before, my modelling is stratified into four age profiles: 0-16, 17-39, 40-64 and 65+. I am personally aware, being in the oldest of these groups, and being very cautious about all contacts, including on public transport, in healthcare settings and shops, that many people across the whole population are also cautious, to a greater or lesser extent.
All calculations in my model are made within those age groups (as well as by variant), even though results are mostly presented in aggregate for the whole population. Serious cases caused by each variant are shown in all charts in the the first two slideshows, and I show charts for particular age groups later on.
The forecasts I will show below should be worst-case as far as the model is concerned, because with the -79.64% NPI effectiveness reduction, the core transmission rate of Covid-19 in the model is not reduced by NPIs or by any modified behaviour by the population.
Vaccination, however, remains. The first recipient (Margaret Keenan) was inoculated on December 8th 2020, and I introduced vaccination to the model from January 1st 2021, when it went into bulk delivery. Incidentally, Ms Keenan has just had her Spring booster (as I have).
It is a testament to the positive impact of the vaccination programme that the epidemic remains fairly well controlled, even with the Government’s aforementioned February 24th 2022 removal of all legal restrictions.
In the model, in the first slideshow, I reflected this by the NPI reduction by 79.64% (which effectively removed all modelled Government mitigations and public behavioural changes).
This maintenance of control of Covid-19 is in contrast to the high rate of increase in modelled cases and deaths I saw in my earlier work in 2020, pre-vaccination, when I reduced NPIs hypothetically in the model to assess the impact.
An early example of such analysis was in my May 14th article, “What if UK lockdown had been 2 weeks earlier” where I explored several levels of reduction in NPIs, as well as looking at outcomes if the UK’s first lockdown were to have been March 9th instead of March 23rd 2020. The differences in cases and deaths outcomes were significant, highlighting the vital importance of NPIs at that time, pre-vaccination.
Other key model parameters
As well as the four age groups, with vaccinations (from zero to three jabs) by age group, the model caters for waning immunity, vaccination hesitation (vac_hes), different variant transmission rates (k11), virulence (fSS) and death rate (fmort), all by variant and age group.
Vaccinations in the model are applied in many sequential stages at different rates (k8, k28 & k38) for the three possible jabs, respectively, following the priorities set by the NHS (National Health Service) from time to time on the advice of the Joint Committee on Vaccination and Immunisation (JCVI).
Efficacy (vac_eff) of vaccination is also set by jab number (1st, 2nd or 3rd) and within age group, with a modifying multiplier var_eff per variant (5 so far), shown in the chart annotations for each variant.
Other key parameters, also set by population group and variant, include:
| Parameter | Model Variable |
| Infection rate per day per person | k1 |
| Infection incubation period in days until Sickness | k2 |
| Half-life in days in Sick until Serious Sickness | k3 |
| Half-life in days in Seriously Sick until Death | k4 |
| Half-life in days until a Sick person become Better | k5 |
| Half-life in days until a Seriously Sick person becomes Better | k6 |
| Half life in days until a Better person is fully Recovered | k7 |
| Daily rate of jabs 1, 2 and 3 | k8, k28 & k38 |
| Immunity waning half-life until Recovered become Susceptible again | ki |
| Vaccination hesitation fraction by population group | vac_hes |
Model structure
The model (an “SIR” style model), which I have developed greatly from an original codebase by Prof Alex de Visscher at Concordia University, comprises “compartments” for each state of health (or otherwise) of a person, with various rates “r” defining the rates per day of transitions between compartments.
These relationships may be seen in the flowchart below, linking all of the compartments with the associated transition rates. When uninfected people are vaccinated, they move across the chart at the top (uninfected) level from U (unvaccinated) to V1, and then to V2 and V3 after successive vaccinations.
Each vaccination status has its own column, modelling the progress of infection status; these columns represent unvaccinated people (the U column), and also those people with one, two or three jabs, in the V1, V2 and V3 columns respectively.
When infected, people transition down those respective columns from Uninfected (U, V1, V2 and V3) to Infected (IU, IV1, IV2 and IV3), Sick (S, SV1, SV2 and SV3), Seriously Sick (SS, SSV1, SSV2 and SSV3), respectively, and from there, either: via Better (BU, BV1, BV2 and BV3), but still infective, to Recovered (RU, RV1, RV2 and RV3); or to Death (D).
After a half-life, defined by the ri rates, representing how long it takes for immunity to wane, spent in the the recovered states RU, RV1, RV2 or RV3, people move back up to the Uninfected (and Susceptible) states U, V1, V2 and V3 respectively, where they can potentially be reinfected, at different rates depending on vaccination status.
All rates r(i,j) in the model and shown in the flowchart below are dependent on vaccination status. Just two of very many scholarly articles published over the last year or moreconfirming this are reported here in the BMJ, and here in The Lancet, showing that vaccination (at different levels) reduces the severity of Covid-19 disease, thus reducing the tendency to serious illness and/or death.
In the flowchart below, j always labels the population group, and i always labels the variant involved. Arrows on the chart indicate the possible transitions, and the “r” rates, in people per day, are derived from the “k” numbers defined in the table above, each r being obtained by multiplying the appropriate k rate by the size of the relevant source compartment (numbers of people in the compartment) on any given day. One day is the time step of the differential equations of the model simulation, and all compartments and variables in the flowchart are in this way time-dependent.

Comparative scenarios for fSS and fmort
I ran options for virulence fSS and mortality fmort for Omicron BA.2, as follows, by applying three different fractional multiples for fSS and two for fmort for Omicron BA.2 compared with Delta. The model has been accurate until Omicron BA.1, but there has been recent divergence for BA.2, especially after the removal of legal NPI restrictions, and so I focused my changes on BA.2 at this stage.
| Scenario | fSS_mult | fSS % | fmort_mult | fmort % |
| UK_894 (base case, as BA.1 compared with Delta) | .3 | 3% | .7 | 1.05% |
| UK_895 | .7 | 7% | .7 | 1.05% |
| UK_896 | 1 | 10% | 1 | 1.5% |
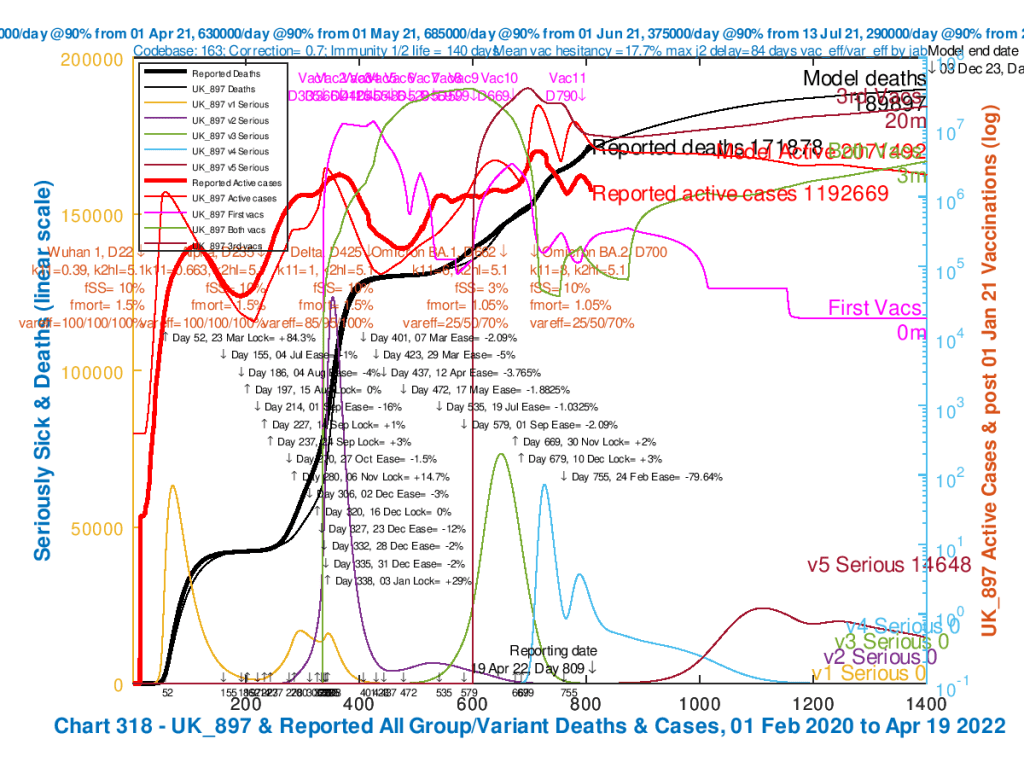
| UK_897 | 1 | 10% | .7 | 1.05% |
| UK_898 | .3 | 3% | 1 | 1.5% |
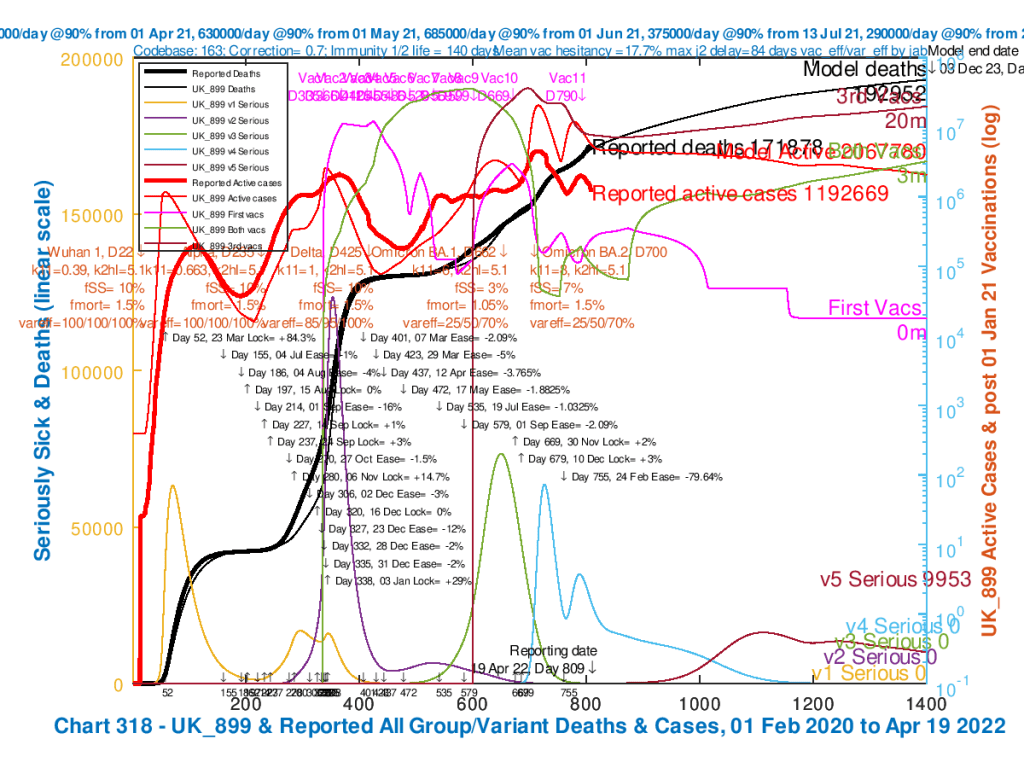
| UK_899 | .7 | 7% | 1 | 1.5% |
Charted outcomes for the fSS (3) and fmort (2) scenarios, 6 in all
Modelled Active Cases at December 3rd 2023 (Day 1400 in the model) are around 2 million in these scenarios, with deaths at around 190,000 depending on scenario. But recall that in these scenarios, all NPIs in the model have been removed on February 24th 2022; the effect is that from this date, not only are there no Government mitigations in the model, but there is also no voluntary self-isolation, mask-wearing or other social distancing. This should be worst-case for each scenario.
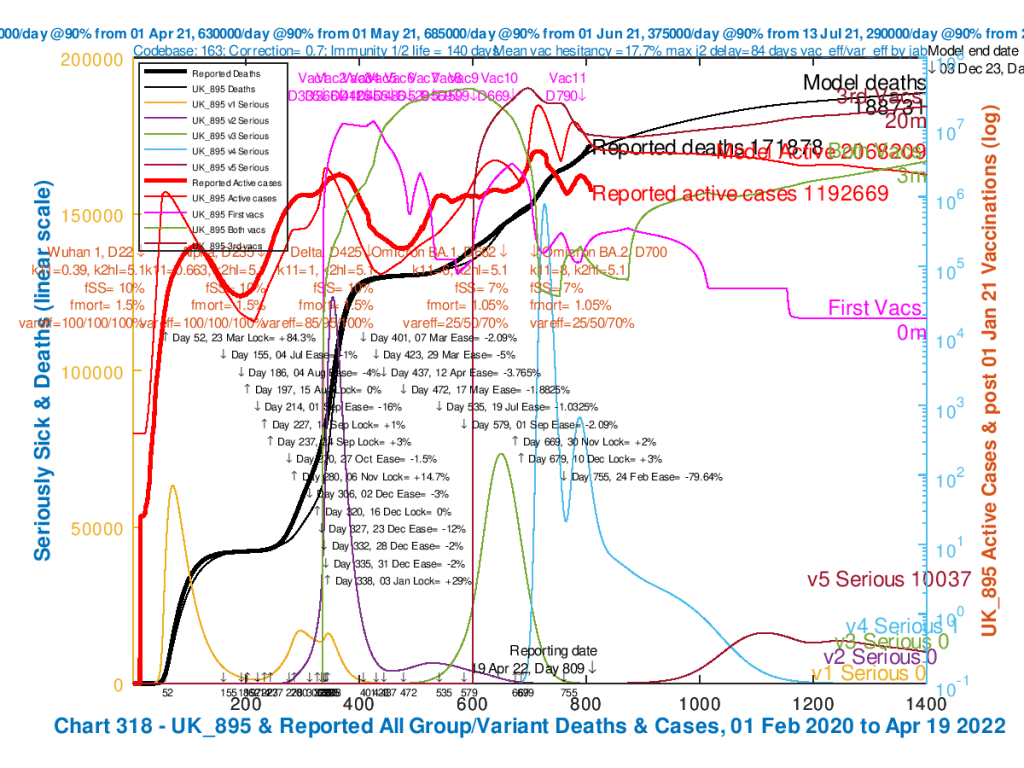
I present the 6 scenario charts as a slideshow for ease of comparison. The heavier red and black curves represent the reported Active Cases and Deaths to April 19th, with the light curves on the chart showing the modelled data.
In all charts 318 in the following slideshow, there are vaccinations for adults from January 1st 2021, and for 5-11 year-olds from April 1st 2022. There is a 24th February NPI with 79.6% reduction. Omicron BA.1 transmission k11 = 6 and BA.2 k11 = 8. Incubation half-life is 5.1 days. var_eff = 25/50/70% depending on Jabs 1, 2 or 3 (booster). Model outcomes for all Active Cases, Modelled serious Cases for 5 variants, and cumulative Deaths are plotted to December 3rd 2023, with Reported Active cases and deaths to 19th April 2022.
Only Omicron BA.1 and BA.2 virulence, fSS and mortality, fmort vary for each chart, as shown in the chart captions.
These scenarios, all with the February 24th NPI at -79.64%, represent worst cases for the virulence and mortality parameters chosen, with only vaccination protecting the population against infection and its consequences after that date. Given that, I was quite surprised in running these scenarios that the increases in infection and deaths outcomes were as limited as they are.
Additionally, because the model only vaccinates uninfected people, vaccinations are reduced in the model when there are higher numbers of infections, compared with model runs in my earlier articles, where there were higher levels of NPIs, reducing infection rates, allowing an increased level of vaccination.
Charted outcomes for 5 NPI scenarios
In this section, I will present variations of the “base case”, UK_994, with lower reductions in the NPI settings to see how the model responds. These runs allow for the NPI effectiveness in the model to represent varying degrees of voluntary precautions on the part of the public. The following table shows the settings (which may also be seen in the annotations for NPIs in the body of the charts).
| Scenario | Intervention % reduction | fSS_mult | fSS % | fmort_mult | fmort % |
| UK_994 (base case) | -79.64% | .3 | 3% | .7 | 1.05% |
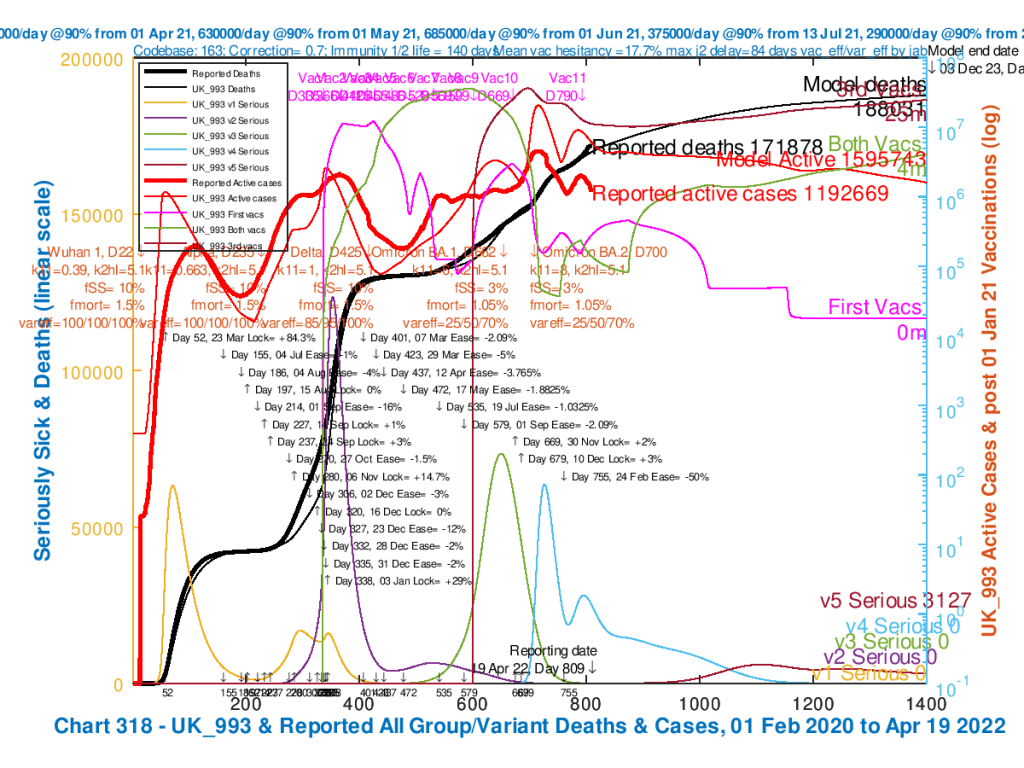
| UK_993 | -50% | .3 | 3% | .7 | 1.05% |
| UK_992 | -30% | .3 | 3% | .7 | 1.05% |
| UK_991 | -15% | .3 | 3% | .7 | 1.05% |
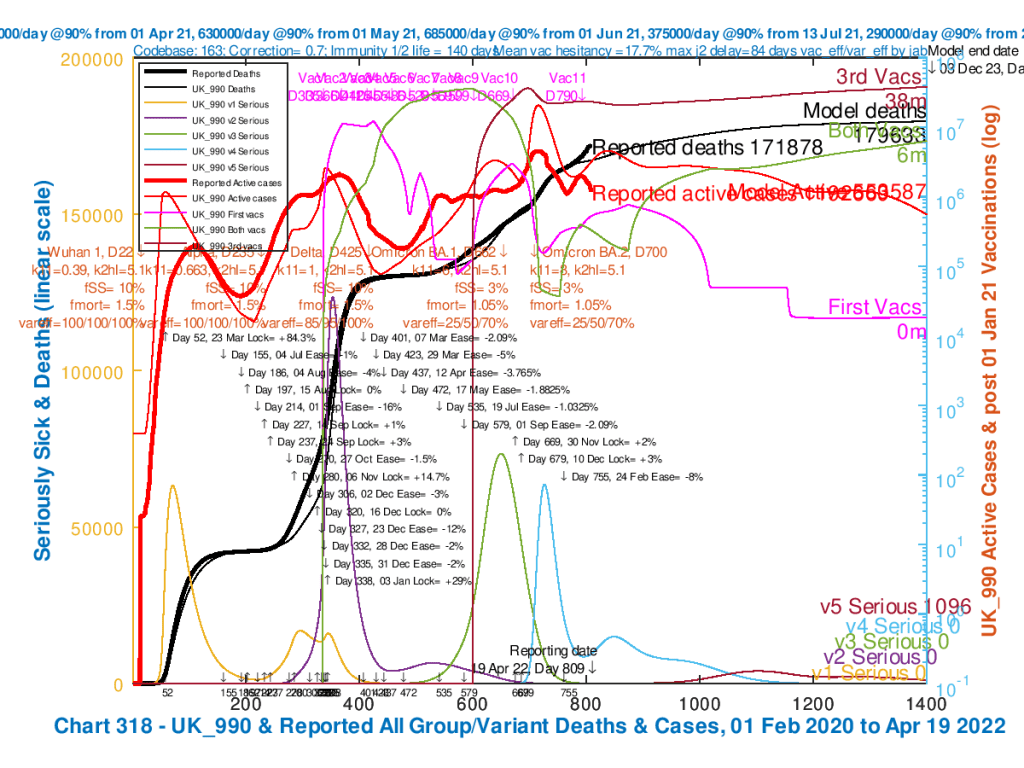
| UK_990 | -8% | .3 | 3% | .7 | 1.05% |
The resulting charts are again shown as a slideshow to enable easier comparison. As we can see, the December 3rd 2023 Active Cases and Deaths reduce along with lower percentage reductions of the NPIs. Vaccination remains, although slightly increased in the scenarios where there are fewer infections, because only uninfected people are vaccinated in the model.
The charts in this slideshow are similar to those in the slideshow above, except that here, fSS=3% and fmort=1.05% for both Omicron variants in all scenarios.
And this time, the 24th February NPI varies in each chart from 8% through 15%, 30% and 50% to 79.64% reduction. The NPIs in each scenario are shown in the chart captions and in the chart body, including the most recent on February 24th which is the only one varying between the scenarios..
We see in these charts that as the February 24th reduction in NPIs is increased from 8%, through 15%, 30% and 50% to a maximum of a 79.64% reduction (which means the removal of all NPIs and voluntary public precautions), the Active Cases and cumulative Deaths at the end of the model period, December 3rd 2023, gradually increase.
At 8% final NPI reduction, Active Cases at Day 1400 (December 2nd 2023) stand at 559,597, and cumulative deaths are 179,663; these rise to 2,063,484 and 190,485, respectively when all NPIs are removed, a 79.64% reduction in NPI effectiveness. That setting for NPIs effectively reverses the cumulative impact of all previous NPIs, along with any public voluntary behavioural precautions.
It is only vaccination that keeps the situation under any kind of control in that context, as I mentioned earlier, something that has consistently been the case ever since I introduced vaccination to the model framework on January 1st 2021. Without vaccination, the removal of NPIs in the model causes Cases and Deaths to increase very rapidly, as I showed in that earlier work.
Shortening the Omicron BA.2 incubation period
I ran one further scenario, UK_995, with a 3.4 day infection incubation period (k2_half_life_v5) for Omicron BA.2, instead of 5.1 days in all the previous scenarios. All other parameters are as for the Scenario UK_994 above.
I did this because I have been exploring such settings as we learn more about Omicron and its actual and potential variants. I will report on Incubation period changes in more detail in a subsequent article, but in the meantime here is the one chart for the scenario UK_995, representing 3.4 days incubation period (reduced from 5.1 days), in the context of the full -79.64% withdrawal of all NPIs on February 24th.

The clear effect of the 3.4 day half-life for the infection incubation period is to reduce the deaths by Day 1400, from 190,486 for the 5.1 days incubation period in Scenario UK_994, shown earlier, to 189,323 in this Scenario UK_995, with 3.4 days incubation, although they are also still increasing in both scenarios at that point. Active cases also reduce by then, from 2,063484 to 1,634,513.
In the model, there is a less obvious (and surprising) effect of the shortening of the Omicron BA.2 infection incubation period to 3.4 days, while leaving Omicron BA.1 at 5.1 days.
At Day 1400, when the BA.2 incubation period is reduced, the 3,228 Seriously Sick cases that remain in Scenario UK_995 at Day 1400 comprise 3,227 Omicron BA.1 serious cases, and just one BA.2 serious case.
This is in contrast with Scenario UK_994 , when the BA.2 Seriously Sick cases were 4,096 at Day 1400, with just one BA.1 serious case. I shall need to take a closer look at that.
The reduction in Active Cases overall in Scenario UK_995 allows cumulative third vaccinations to increase from 20 million to 24 million, as the model only vaccinates uninfected people.
This isn’t entirely realistic, as often, in real life, because of asymptomatic infection, such infected people are also vaccinated, because neither the recipient nor the vaccination centre necessarily knows that an asymptomatic person is infected. But I hesitate to model this effect, as it would be difficult, if not impossible, to source real reported data on it.
Age-related charts
I mentioned before that all calculations in the model are done within age-groups, and then aggregated for presentation. Here I show four age-related charts, for completeness. Note that in these four age-group charts, Serious Cases are aggregated and not shown for each variant separately, as the aim is to highlight the age-related differences in outcomes for All Cases, Infections (Active Cases), All Serious Cases and cumulative Deaths.
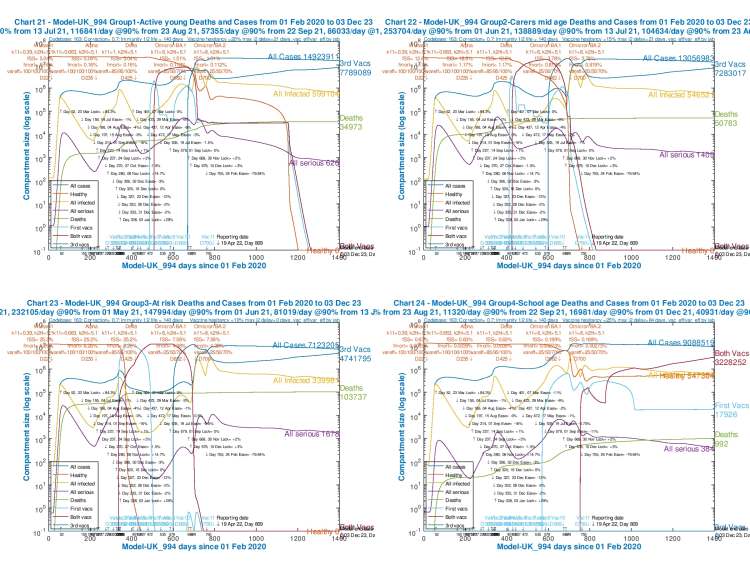
Note that as we would expect, death rates increase with age, but for infections (cases), there are proportionately far more in the younger age groups, partly because they were later in receiving vaccinations, as can be seen in the charts, and partly because younger age groups socialise and/or work more.
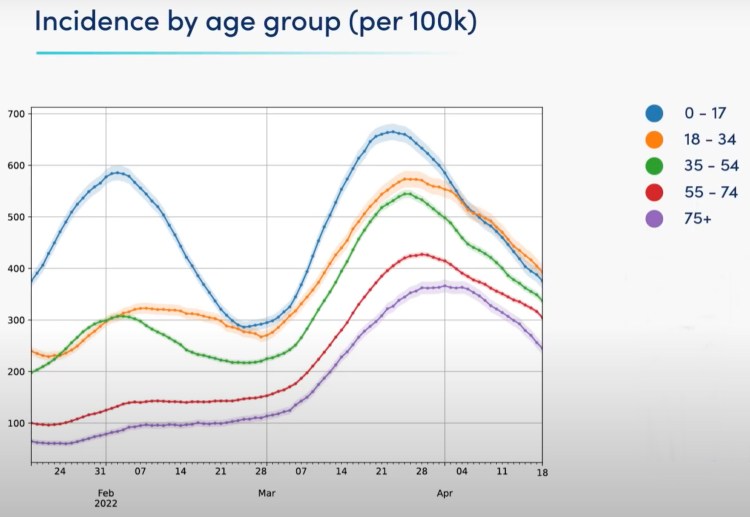
The differences in age-related rate of infection can be seen below in the ZOE Project’s comparison of 2022 age-group case incidence of new cases, confirming that the overall incidence rate per 100,000 is driven by younger age groups, with the over-75’s showing the lowest rate, no doubt thanks to the high take-up of vaccination in the UK for that age-group, who were also the earliest to be inoculated at the beginning of 2021, and then to receive their boosters.
NB the ZOE analysis is for five age groups, rather than the four that I use.
Discussion
It is evident from all of the charts that while Active Cases start to reduce, and are still declining by the end of the forecasting period (December 2nd 2023), albeit with the wave behaviour and honeymoon period I mentioned last time, deaths continue to increase, but at a reduced rate.
Covid-19 is still active at that point, fairly well controlled by vaccination, even in the absence of legally enforceable NPIs. Whether public behaviour will continue to limit infection rates to some extent remains to be seen.
Most experts and commentators seem to think that the SARS-Cov-2 pandemic will have become endemic by then (if it hasn’t already, as we are encouraged to “live with the virus”).
If the current rate of infections and deaths were to have been experienced a year or two years ago, I think we would have been more worried then than we seem to be at the moment.
What is noticeable from the modelling is that that successive variants that have become dominant have been increasing significantly in transmission rates, and my expectation would be that next one will probably need to be even more transmissive than Omicron BA.2 to become dominant. I shall look in more detail at Tom Wenseleer’s work, mentioned above,
The impact of an infectious disease on the human population is a complex derivative of varying human susceptibility and of several of the key virus characteristics, not just its transmission rate, but also its virulence (infectivity, or tendency to cause illness) and mortality (tendency to kill people).
There is no “intelligent design” involved, although commentators sometimes talk as if a virus designs itself to compete more effectively. It’s a matter of natural selection, of course. When the combination of those human and virus factors allows the virus to infect plenty of people, it helps the spread of infection if those people survive and remain infective somewhat longer. Crudely put, if it kills people too soon, it’s bad for the virus business.
Eventually, as more people become infected, and/or are vaccinated (and evidence supports that it more effective to have both, as long as what infects you doesn’t kill you) then the virus runs out of people to infect, although Omicron seems more able to re-infect people than previous variants.
Concluding comments
Even allowing for model idiosyncrasies (a polite word for errors), the outcomes across the various parametric runs indicate consistently that infections and deaths will continue, albeit at reducing rates, thanks to vaccination, when NPIs are withdrawn.
I hope not to have to add another major variant to the UK model (but NB the Wenseleer South Africa warning about further Omicron BA.x variants, which would change that picture) and therefore not to have to develop the model and add to my blog as frequently as I have in 2020 and 2021.
It is still an uncertain Coronavirus world out there. Models can help forecast the future, but models are never perfect and are always being refined, as mine has over the last two years or more.
My modelling at present continues to confirm the vital importance of vaccination. When I have discussed the pandemic with several experts in the field, they have all made sure to advise me to take vaccination when offered.







One thought on “They think it’s all over – but it isn’t – Coronavirus”