Cambridge Conversations video
In my post a few days ago at https://www.briansutton.uk/?p=1536, I mentioned that the webinar I reported there was to be released on YouTube this week, and it is now available.
It is VERY much worth 40 minutes of your time to take a look.
The potential cyclical behaviour described there is one that, as we see, the Imperial group under Neil Ferguson have been looking at; and the Harvard outlook seems similar, well into 2021, and as far as 2022 in the Harvard forecasting period.

It seems likely, (as Imperial have been advising the UK Government) from the recent daily updates, that Government is preparing us for this, and have been setting the conversation about any reduction in the lockdown clearly in the context of avoiding a further peak (or more peaks) in infection rates.
Alex de Visscher’s model I have been working with (I described it at https://www.briansutton.uk/?p=1455 ), and other similar “single-phase” models, would need some kind of iterative loop to model such a situation, something entirely feasible, although requiring many assumptions about re-infection rates, the nature and timings of any interventions Government might choose to relax and/or add, and so on. It’s a much more uncertain modelling task than even the work I’ve been doing so far.
Model refinement
Inasmuch as I have been looking at the fit of my current UK model to the daily data (see https://www.briansutton.uk/?p=1571), it was clear that the model was approaching a critical period over the next couple of weeks: UK death data, and to some extent the daily number of cases was levelling out, such that I could see that my model (predicting c. 39,000 deaths) was ahead of what might be likely to happen.
The modelled pandemic growth rates depend on many data, and two parameters – the time it takes for a person to infect another (i.e. the initial rate of infection per day, k11=0.39 in the current model), and also the intervention effectiveness parameter (how well the social distancing is working at reducing that infection rate per day), interv_success, set at 85% in the current model – are pertinent to the shape of the growth from the intervention date.
Since the lockdown measures are critical to that infection rate outcome as we go forward, yesterday I decided to run the model with interv_success set at 90%, and indeed it did bring down the predicted death outcome to c. 29,000. Here are those new charts, one with linear axes, and the other with logarithmic (log10) y-axis:


These charts match the reported deaths data so far a little better; but for case numbers (a harder and more uncertain number to measure, and to model) with 90% intervention effectiveness, the reported data begins to exceed the model prediction, as we see below. This effect was enhanced by the weekend’s lower UK reported daily figures (April 18th-20th), but the April 21st figure showed another increase. It’s probably still a little to early to be axiomatic about this parameter, and the later section on model sensitivity explains why.
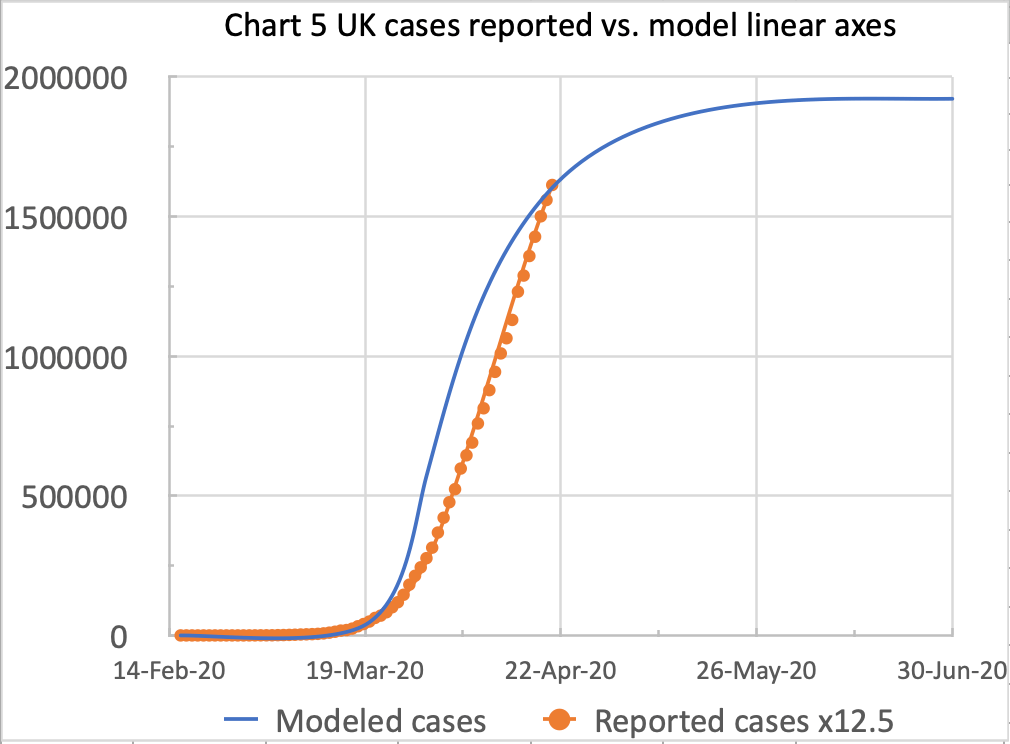
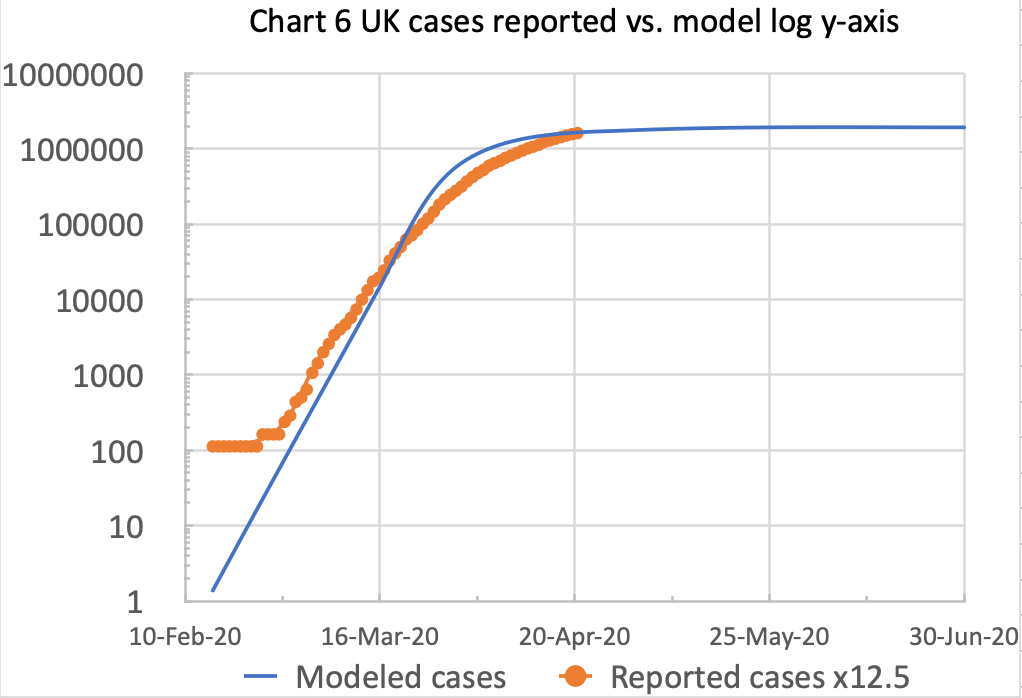
The two original charts for cases, with the 85% effectiveness, had looked likely to be a better match, going forward, as we seem to be entering a levelling-off period:


We can see that the model is quite sensitive to this assumption of intervention effectiveness. All data assumptions at an early stage in the exponential growth of pandemics are similarly sensitive, owing to the way that day-on-day growth rates work. The timing of the start of interventions (March 23rd in the case of the UK) and also, as we see below, the % effectiveness assumption both have a big effect.
Model sensitivities
This highlights the need to be cautious about adjusting lockdown measures (either in real life or in the models), until we can be sure what the likely impact of the “intervention effectiveness” percentage will be, and how this affects the outlook. Here we see two base-case sensitivity charts from Alex’s original paper at https://arxiv.org/pdf/2003.08824.pdf
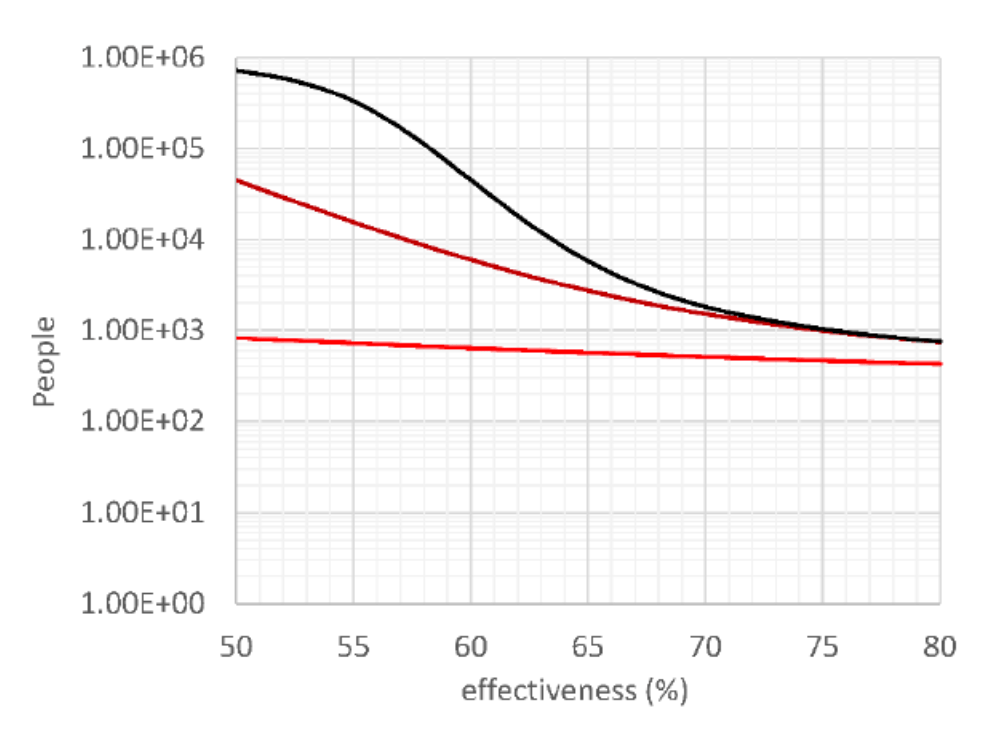
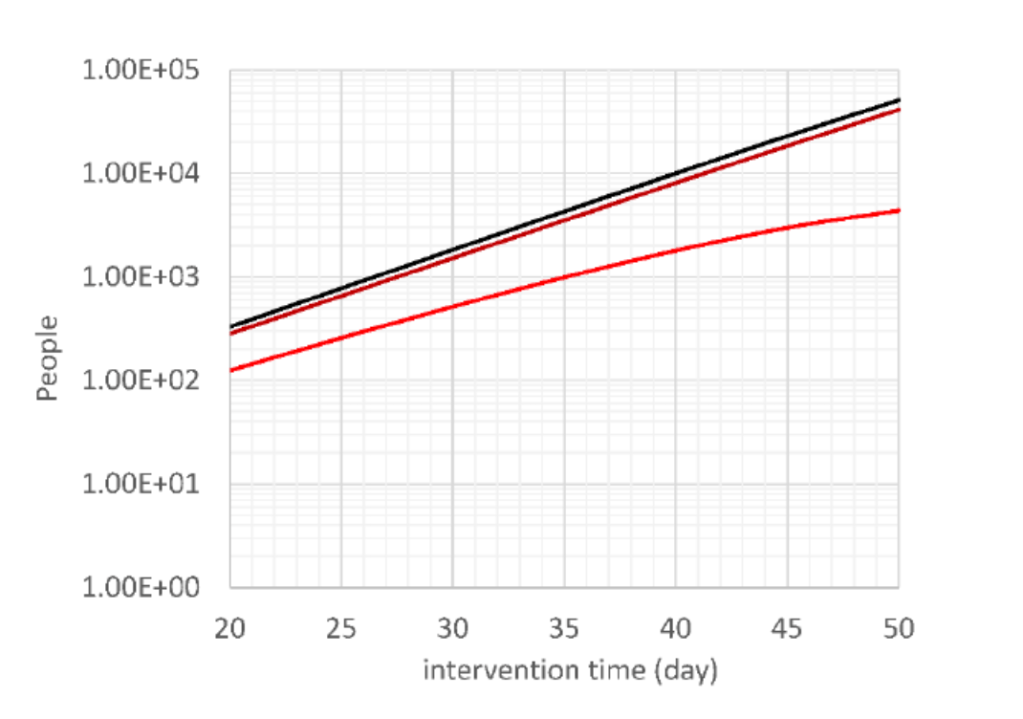
These are generic logarithmic charts from his base model. On the left, we see the number of deaths after 60 days (bright red), 150 days (dark red) and 300 days (black) versus % effectiveness of intervention, for the base case of the (then) typical (outside China) doubling time 4 days, with intervention on day 30 (in the UK it (the lockdown) was on Day 51, March 23rd).
On the right, we see the number of deaths after 60 days (bright red), 150 days (dark red) and 300 days (black) versus the time of intervention, for the base case, doubling time 4 days, and intervention effectiveness 70 %.
Since the UK intervention on March 23rd, I feel that the intervention effectiveness has been quite good overall, so 85% and 90% don’t seem unreasonable options for the UK model.
For our UK intervention timing, the jury is out as to whether this was too late, or if an earlier intervention might have seen poorer compliance (effectiveness). The Government made the case (based on behavioural science, I believe) that the UK public would tire of lockdown, and therefore wanted to save lockdown for when they felt it would really be needed, to have its maximum effect nearer to when any peak in cases might have swamped the NHS.
The point in this section is to illustrate the sensitivity of outcomes to earlier choices of actions, modelled by such mathematical models; such models being the basis of some of the scientific advice to the UK Government (and other Governments).
Epidemic decline and multiple peak issues
A full discussion of the following points can be seen in Alex’s paper at https://arxiv.org/pdf/2003.08824.pdf
Alex had run his generic model (population 100m, with 100 infected, 10 sick and 1 seriously sick on day 1) for a couple of scenarios, in slow, medium and fast growth modes: one, that represented a “herd immunity approach” (which turns out not to be effective unless there is already a pharmaceutical treatment to reduce the number of infective people); and two, a “flattening the curve” approach, which modelled reducing the infectivity, but NOT controlling the disease (i.e. R0 still well above 1), which delays the peak, but still swamps the healthcare system, and allows very large numbers (about 2/3 of the base model numbers) of deaths.
This must have been the kind of advice the UK Government were getting in mid-March, because these approaches were demoted as the principal mechanisms in the UK (no more talk of herd immunity), in favour of the lockdown intervention on March 23rd.
What next after lockdown?
The following charts (from Alex’s paper) show the outcomes, in this generic case, for an intervention (in the form of a lockdown) around day 30 of the epidemic.
Starting from the base case, it is assumed that drastic social distancing measures are taken on day 30 that reduce R0 to below 1. It is assumed that the value of k11 (the starting infectivity) is reduced by 70 % (i.e., from 0.25 per day to 0.075 per day, equivalent to R0 decreasing from 2.82 to 0.85).

On the left chart, we see: Uninfected (black), all Infected (blue) and Deceased (red) people versus time. Base case, doubling time 4 days, intervention on day 30 with 70 % effectiveness.
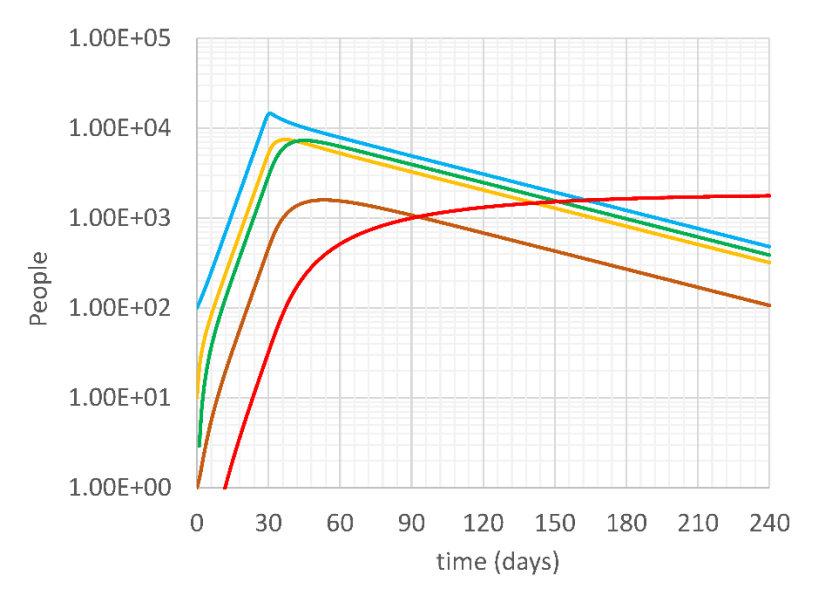
On the right chart, we see Incubating (blue), Sick (yellow), Seriously Sick (brown), Recovering (green) and Deceased (red) people versus time. Base case, doubling time 4 days, intervention on day 30 with 70 % effectiveness.
Conclusions for lockdown
What is clear from these charts is that the decline of an epidemic is MUCH slower than its growth.
This has important repercussions for any public health policy aiming to save lives. Even seven months into this generic modelled intervention, the number of infected is comparable to the number of infected two and a half weeks before the intervention.
On the basis of these simulations, terminating the intervention would immediately relaunch the epidemic. The intervention would need to be maintained until the population can be vaccinated on a large scale.
This difficulty is at the heart of the debate right now about how and when UK (or any) lockdown might be eased.
This debate is also conducted in the light of the Imperial and Harvard modelling concerning the cyclical behaviour of the epidemic in response to periodic and partial relaxations of the lockdown.
This is where the two parts of the discussion in this blog post come together.

8 thoughts on “Cambridge Conversations and Coronavirus model refinement”